Funding of £20 million will support scientists to develop and test innovative medical treatments and diagnostic tools using the latest advances in quantum, robot technology and imaging.
A further investment of £16.5 million in new digital health hubs across England will promote knowledge and skills sharing across a range of partners including:
- the NHS
- social care providers
- universities
- businesses
New healthcare technologies
Five projects will create healthcare technologies for the future supported by the Engineering and Physical Sciences Research Council (EPSRC), with £2 million funding from the Medical Research Council (MRC).
They will develop:
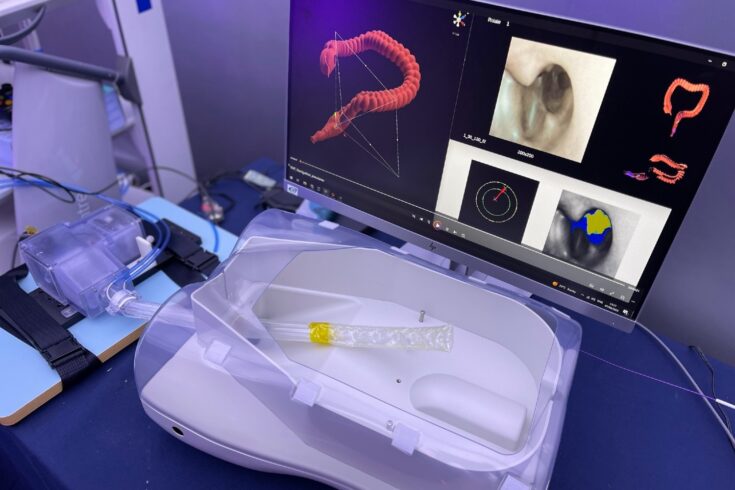
Self-propelled robot endoscopes
Endoscopes are tube shaped instruments that can film procedures inside the body.
Self-propelled robot endoscopes, being developed by scientists at Imperial College London, aim to move seamlessly and carry miniature surgical lasers and powerful tissue analysis.
This one-stop device will have ability to find and treat early gut cancer, reducing the need for further surgery.
An innovative way of managing diseases using low intensity ultrasound
Scientists at the University of Oxford will use the exciting new development of microbubbles as image contrasting agents which can be stimulated using the light of ultrasound.
The treatment could be used to manage diseases such as:
- cancer
- stroke
- Alzheimer’s disease
- drug resistant infections
Digital twin assisted surgery
Digital twins, or exact computer models, of patients will be used by doctors to test procedures and predict outcomes, enabling doctors to adapt and personalise the treatment for each patient.
University of Strathclyde researchers believe this will significantly improve patient outcomes and recovery times.
Portable brain imaging for stroke patients
Scientists at Imperial College London will develop a portable brain imaging ultrasound tool that can diagnose and treat neurological conditions such as stroke.
The technology uses advanced computer modelling to remove distortions producing a high resolution, high contrast image of the brain.
It will enable ultrasound to be used successfully for the first time.
Computer engineered models of leukaemia to better predict the disease and improve drug screening pathways
Scientists at the University of Glasgow will develop a way of detecting leukaemia many years before cells become malignant.
They will use developments in the field of methanobiology, the process of detecting very early cellular changes in the body.
Digital health hubs
A further £16.5 million will support new digital health hubs across England that will drive the development of innovative digital technologies for healthcare.
They will promote knowledge and skills sharing across healthcare, academia and business, and drive innovation in digital health.
The hubs will be led by the universities of:
- Bristol
- Newcastle
- Sheffield
- University College London
- King’s College London
They will focus on five key healthcare challenges:
- antimicrobial resistance
- health and care outside hospital and disease prediction, diagnosis and intervention
- tackling health inequalities by developing digital healthcare technologies to the point of use in the NHS
- addressing the unmet health needs of underserved communities, and digital exclusion
- development of digital technologies such as symptom tracking apps or wearable devices to improve health
Investing in new technologies
Dr Kedar Pandya, Executive Director of Cross-Council Programmes at EPSRC, said:
The projects and hubs announced today will deliver a variety of innovative approaches to improve healthcare outcomes for patients.
This investment will support scientists and engineers who are transforming the way we treat and diagnose diseases by using the latest developments in robotics, computer modelling and imaging.
Further information
Digital health hubs projects
Funding of £16.5 million from EPSRC and the ‘securing better health ageing and wellbeing’ and ‘tackling infections’ UK Research and Innovation strategic themes.
EPSRC Digital Health Hub for Antimicrobial Resistance (AMR)
Professor Rachel McKendry, University College London
The Digital Health Hub for antimicrobial resistance (AMR) aims to harness innovative digital technologies to ultimately transform antimicrobial one-health surveillance and antimicrobial stewardship, recognising the interconnectedness of AMR between humans, animals and the environment.
This hub will bring together a critical mass of researchers working across traditional disciplines, including:
- computer science
- data visualisation
- biomedical engineering
- behavioural science
- environmental science
- clinical and public health research
The researchers will work with the NHS, UK Health Security Agency, Centre for Ecology and Hydrology, charities and industry partners.
We aim to nurture cross-sector partnerships to grow a network of excellence, to engineer digital health technologies and to upskill 100 researchers to become future leaders.
Leadership Engagement Acceleration and Partnership (LEAP)
Professor Ian Craddock, University of Bristol
The LEAP Digital Health Hub is a partnership of:
- the south-west’s leading universities
- more than 20 supporting companies
- NHS Trusts and Health Boards
- four social care organisations
- the region’s local authorities
- the West of England Academic Health Science Network
- the award-winning business incubator SETsquared
- Health Data Research UK
The hub will address the professional training needs of industry, health and social care providers and academia.
This is proposed to be the world’s largest digital health taught programmes.
The South Yorkshire Digital Health Hub
Professor Tim Chico, The University of Sheffield
The South Yorkshire Digital Health Hub covers a region of 1.4 million people affected by high levels of disease and health inequalities.
It includes:
- all regional NHS organisations including:
- GPs
- adult and children’s hospitals
- mental health services
- the recently introduced South Yorkshire ’Integrated Care System’
- researchers from The University of Sheffield and Sheffield Hallam University
- large and small companies
- patient and public groups
These partners between them have all the necessary expertise and experience in developing new digital health technologies to the point of use in the NHS.
The hub will offer specialist health training for researchers, clinicians, patients and the public, made freely available through YouTube.
Northern Health Futures (NortHFutures) Hub
Professor Abigail Durrant, Newcastle University
NortHFutures is envisioned as a world-leading healthcare technology (health-tech) innovation ecosystem.
Based in the north-east and north Cumbria (NENC) region, the hub:
- involves six universities:
- Cumbria
- Durham
- Newcastle
- Sunderland
- Teesside
- Northumbria
- partners with:
- NHS Trusts and NENC Integrated Care Board
- local authorities
- industry
- voluntary, community and social enterprise, across NENC, UK, and globally
NortHFutures humanises health-tech; equity, participation, and investment in people is core for interconnecting diverse stakeholders.
NortHFutures will address underserved communities to stimulate socio-economic and cultural growth.
Through our human- and civic-centred approach, we will develop resources for populations of all ages to invest in their possible futures.
King’s Health Partner (KHP) Digital Health Hub
Professor Sebastien Ourselin, King’s College London
Digital health technologies such as symptom tracking apps or wearable devices that monitor heart rate, activity or sleep patterns can make a positive difference to the outcomes of patient treatment, management and care.
The KHP Digital Health Hub will enable the development of new digital technologies and reduce the time it takes for these to benefit patients.
By providing expertise, partnerships with industry, and a physical location for technology developers to work together this project will enable new businesses to:
- grow rapidly
- increase the availability of digital health technologies nationally
- make a more immediate difference to patients’ lives
Transformative healthcare technologies
Investment of £20 million from EPSRC and MRC.
Exploiting mechanobiology to interrogate the cellular state
Professor Manuel Salmeron-Sanchez, University of Glasgow
Leukaemia kills more than 300,000 people in the world every year.
The evolution of the disease happens as we get older, but there is now evidence that cells in our body progress towards becoming malignant many years before they can be identified with current diagnostic techniques.
This project will exploit mechanobiology, a field of research that has progressed in the last 10 years, as a novel method to identify very early changes in cellular state and to detect cancer earlier than before.
Engineering precision medicine for the 21st century
Professor Eleanor Stride, University of Oxford
The UK is facing a care crisis due to its ageing population and the increase in diseases such as cancer, stroke, Alzheimer’s and drug resistant infections, whose prevalence increases with age.
Better therapeutic solutions are urgently needed to manage these conditions, prevent premature deaths, enable patients to continue living independently and ease the burden on care providers.
The aim of this research is to bring together scientists from the disparate fields of quantum physics and pharmaceutical chemistry with biomedical engineers, immunologists, and clinicians to find solutions.
The approach is based upon the exciting new finding that microbubbles, currently used as imaging contrast agents, can be stimulated with low intensity ultrasound to produce light.
This will offer a unique method for delivery of targeted therapies.
Transforming early diagnosis and treatment of gut cancers
Professor Ferdinando Rodriguez y Baena, Imperial College London
This research aims to transform early diagnosis and treatment of gut cancers using flexible endoscopy.
A soft robotic endoscope with a probe carrying a miniature surgical laser, and a powerful tissue analysis device will be combined.
This automated device will be easier to use than standard endoscopes and will allow endoscopists with less experience to perform the surgery.
The ability to find and treat early tumours will:
- reduce the number of patients requiring further surgery
- reduce discomfort
- lower the number of tumours that grow back
Automation of key steps of the test, including deployment of the instrument, detection of cancer, and laser surgery, that will eventually allow cancer surgeries to be done in outpatient clinics or GP surgeries.
Real-time digital twin assisted surgery (DTAS)
Professor Will Shu, University of Strathclyde
There is a clear clinical need for minimising surgical operations, healthcare costs, patient waiting lists, and associated patient complications.
To address this need, the aim is to digitally transform future surgery, particularly for cancer, by creating a ground-breaking real-time DTAS technology.
The patient is at the core of this technology, with significant and measurable benefits for their quality of life and healthcare.
DTAS can be applied to several types of surgery (open, minimally invasive, or robotic surgery), for high precision tumour removal even in a partial organ resection.
A parallel goal is to revolutionise surgical training, offering a new paradigm of patient-centred personalised surgical rehearsal.
Imaging the brain with ultrasound full-waveform inversion
Professor Mike Warner, Imperial College London
Rapid brain imaging is central to the diagnosis and treatment of acute neurological conditions such as stroke or head trauma.
Existing imaging methods require large, immobile, high-power instruments that are near-impossible to deploy outside specialised environments, leading to unnecessarily delayed diagnosis and treatment, and higher fatality rates.
This project will create a device that can be simply and rapidly applied to any patient, any time, any place, exploiting advances that have already revolutionised imaging in geophysics.
The brain will be imaged using ultrasound waves, transmitted across the head, applying advanced computer modelling to remove the distorting effects of the skull.
This will enable high-resolution high-contrast imaging of the brain unachievable by conventional ultrasound.
Top image: A self-propelled robot endoscope that can film medical procedures inside the body. Credit: Imperial College London