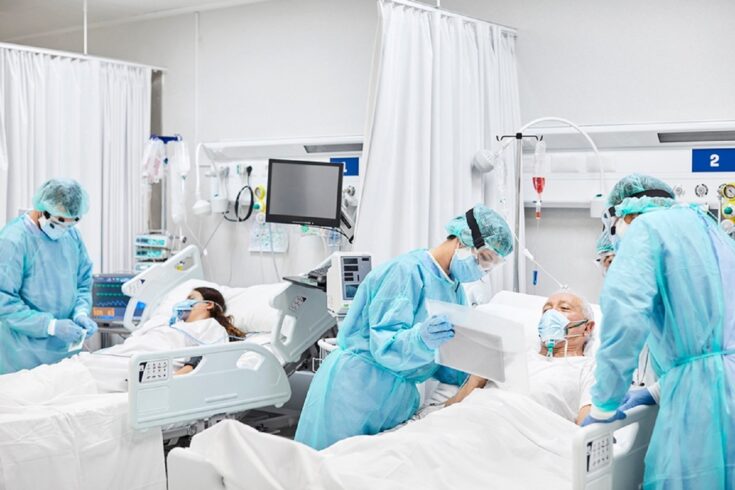
People admitted to hospital with COVID-19 can be divided into four distinct groups, according to data from the world’s largest study of patients with the disease.
Researchers used clinical information and tests carried out on arrival at hospital to predict the patients’ risk of death, ranging from low to very high.
The COVID-19 risk identification tool is helping clinical staff choose the best course of treatment for patients admitted to hospital.
It was built by the ISARIC Coronavirus Clinical Characterisation Consortium, involving researchers from the universities of Edinburgh, Glasgow and Liverpool, and Imperial College London.
The project was funded by UKRI and the Department of Health and Social Care through the National Institute for Health Research, part of the UK government’s COVID-19 rapid research response.
Predicting risk
The ISARIC researchers used data from 35,000 patients admitted to hospital between February and May 2020 who met the criteria for one of the four groups.
The tool was tested and its accuracy confirmed using data from a further 22,000 patients hospitalised from the end of May to the end of June 2020.
Data was used to identify which group a person falls into, and therefore their risk of dying. Data included age, sex, the number of pre-existing conditions, respiratory rate on admission and the results of two blood tests.
One in every 100 patients in the low-risk group was found to be at risk of dying.
That number was 10 in 100 patients in the intermediate-risk group, 31 in 100 in the high-risk group and 62 in 100 in the very high-risk group.
The first accurate risk tool for COVID-19
The categorisations made new treatment pathways possible, the researchers said.
People who fall into low-risk subgroups could be treated at home, while those in the high or very high-risk groups could have more aggressive treatment like early admission to critical care.
This was the first accurate risk tool for COVID-19 patients. Existing tools for pneumonia or sepsis did not offer accurate predictions due to the differences between diseases.
One limitation of the new tool was that it can only be used on hospital patients, and not within the community.
See the published findings in the British Medical Journal (BMJ).
Women under 50 have worse long-term outcomes
ISARIC’s data has continued to shed light on who is worst-affected by COVID-19.
In early 2021, a study showed women under 50 and those who had experienced severe disease had worse long-term outcomes.
Female participants under the age of 50 years old were:
- five times less likely to report feeling fully recovered
- twice as likely to report worse fatigue
- seven times more likely to be more breathless and were
- more likely to have worsening difficulties or a new disabilities, especially relating to:
- memory
- mobility
- communication
- vision
- hearing
- self-care.
Dr Janet Scott, from the MRC-University of Glasgow Centre for Virus Research, lead author of the study, said:
The fact that women under the age of 50 are the group with the worst outcomes could have profound implications for pandemic policy decisions, as well as vaccination strategy.
Discouraging use of antibiotics
ISARIC scientists also reported that the use of antibiotics to treat COVID-19 during the first wave was “very high”, despite bacterial infection being uncommon.
The study was published in The Lancet Microbe and was conducted in collaboration with the Universities of Edinburgh and Liverpool and Imperial College London. It found that 85% of COVID-19 patients received one or more antibiotics during their hospital admission, with the highest use in critical care. 37% of patients were prescribed antibiotics prior to admission.
The over-prescription of antibiotics raises concern about the potential impact on antimicrobial resistance globally.
The ISARIC study is the first detailed understanding of the prescription of antibiotics to COVID-19 patients, and any bacterial co-infections.
Dr Antonia Ho, lead author of the study from the MRC-University of Glasgow Centre for Virus Research, said:
While some COVID-19 patients will require antibiotics, mostly for secondary infections which develop after admission to hospital, our data shows that not all COVID-19 patients should be prescribed antibiotics.
Prof Calum Semple, Co-Lead of the study said,
We only have safe surgery and medical cures for many life-threatening conditions because antibiotics were discovered and mostly still work.
Overuse of antibiotics needs to be avoided to prevent emergence of resistance. When the current threat from COVID-19 subsides, the problem of antimicrobial resistance will remain a threat.
Additional information
ISARIC is a federation of 55 research networks spanning 111 countries. The networks generate the evidence for improving clinical care and responses to infectious disease epidemics. They also support the development and evaluation of new diagnostics, treatments and vaccines.
In 2009, outbreaks like the H1N1 swine flu pandemic showed that cross-border coordination is vital to improve clinical and public health responses to rapidly-emerging infectious diseases.
The Medical Research Council (MRC) provided initial seed funding to establish ISARIC, and in 2011 it gained funding from:
- MRC
- Institut National de la Santé et de la Recherche Médicale (INSERM)
- the Bill and Melinda Gates Foundation
- the Wellcome Trust.
ISARIC’s protocols and infrastructure have been instrumental in the global response to COVID-19. The RECOVERY trial is just one example.
Last updated: 11 November 2021